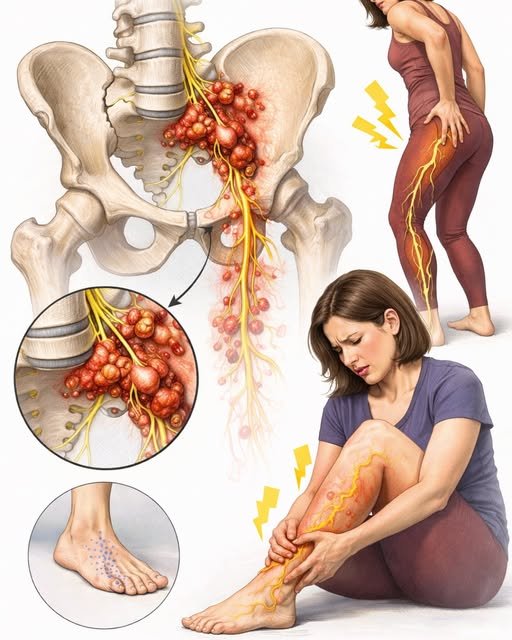
Endometriosis on the Spinal Cord: What You Need to Know
Endometriosis is a condition where tissue similar to the lining of the uterus grows outside the uterus, often causing pain, inflammation, and fertility issues. While it most commonly affects the pelvis, ovaries, and fallopian tubes, in extremely rare cases, endometriosis can involve the spinal cord or surrounding nerves. This condition, known as spinal or neurological endometriosis, can have significant consequences if not recognized and treated promptly.
Understanding Endometriosis
What Happens in Endometriosis?
-
Endometrial-like tissue grows outside the uterus.
-
This tissue responds to hormonal cycles, leading to bleeding, inflammation, and scar tissue formation.
-
Common sites include the ovaries, pelvic lining, bladder, and intestines.
Rarely Affected Areas
-
The spinal cord and peripheral nerves can be affected, though this is extremely uncommon.
-
When it occurs, the growth may lead to neurological symptoms due to compression or irritation of spinal structures.
How Endometriosis Can Affect the Spinal Cord
Mechanisms
-
Direct Spread
-
Endometrial tissue may migrate through blood vessels or lymphatic channels.
-
-
Nerve Involvement
-
Lesions may form near nerve roots, causing radicular pain or neurological deficits.
-
-
Scar Tissue Formation
-
Adhesions can compress the spinal cord or nerve roots, leading to chronic symptoms.
-
Symptoms of Spinal Endometriosis
-
Back pain that worsens cyclically with the menstrual cycle
-
Numbness or tingling in the legs or lower body
-
Weakness or difficulty walking
-
Bladder or bowel dysfunction
-
Sciatica-like pain radiating from the spine to the legs
These symptoms are often mistaken for herniated discs, spinal stenosis, or other neurological disorders, making diagnosis challenging.
Diagnosis
1. Clinical Evaluation
-
Detailed medical history, including menstrual cycle patterns and pain correlation
-
Physical and neurological exams to assess strength, reflexes, and sensation
2. Imaging Studies
-
MRI (Magnetic Resonance Imaging): Most effective for detecting lesions near the spinal cord
-
CT Scan: Useful for evaluating bony involvement
-
Ultrasound: Limited use but can identify adjacent pelvic lesions
3. Biopsy
-
In rare cases, surgical biopsy may be necessary to confirm endometriosis in spinal tissue.
Treatment Options
1. Medications
-
Hormonal therapies: Birth control pills, GnRH agonists, or progesterone can suppress endometrial growth.
-
Pain management: NSAIDs or other analgesics to manage chronic pain.
2. Surgery
-
Laminectomy or lesion excision may be required to remove endometrial tissue compressing the spinal cord or nerves.
-
Minimally invasive approaches are preferred when possible to reduce complications.
3. Rehabilitation
-
Physical therapy and neurological rehabilitation can help restore mobility and function post-surgery.
Prognosis
-
With timely diagnosis and treatment, many patients experience pain relief and improved function.
-
Delayed diagnosis can lead to permanent nerve damage or mobility issues.
-
Close monitoring by gynecologists and neurologists is essential for optimal outcomes.
Frequently Asked Questions
Q: How common is spinal endometriosis?
A: It is extremely rare. Most endometriosis cases are confined to the pelvis. Fewer than 1% of patients experience spinal involvement.
Q: Can spinal endometriosis cause paralysis?
A: In severe cases, compression of the spinal cord may lead to partial weakness or neurological deficits, but full paralysis is rare.
Q: Is surgery always required?
A: Not always. Hormonal therapy can control symptoms in some patients, but surgery may be necessary if lesions compress nerves or spinal structures.
Q: Can endometriosis return after treatment?
A: Yes, recurrence is possible. Long-term management and monitoring are important.
Practical Advice for Patients
-
Track Symptoms with Menstrual Cycles
-
Note any cyclical pain, weakness, or numbness that coincides with menstruation.
-
-
Seek Multidisciplinary Care
-
Gynecologists, neurologists, and neurosurgeons should collaborate for diagnosis and treatment.
-
-
Early Intervention is Key
-
Don’t ignore back pain or neurological symptoms—early imaging can prevent long-term damage.
-
-
Lifestyle Adjustments
-
Gentle exercise, posture care, and pain management strategies can improve quality of life.
-
Conclusion
While spinal endometriosis is extremely rare, its impact can be serious due to the involvement of the spinal cord and nerves. Awareness of cyclical back pain, neurological symptoms, and bladder or bowel changes is critical for early diagnosis.
With timely medical intervention, appropriate medication, and sometimes surgery, patients can achieve symptom relief and maintain mobility. Multidisciplinary care and ongoing monitoring remain essential for optimal outcomes.
✅ Call to Action
-
If you experience cyclical back pain, leg numbness, or urinary changes, consult a gynecologist and neurologist promptly.
-
Maintain a detailed symptom diary to help doctors track patterns.
-
Share this information to raise awareness about this rare but serious form of endometriosis.