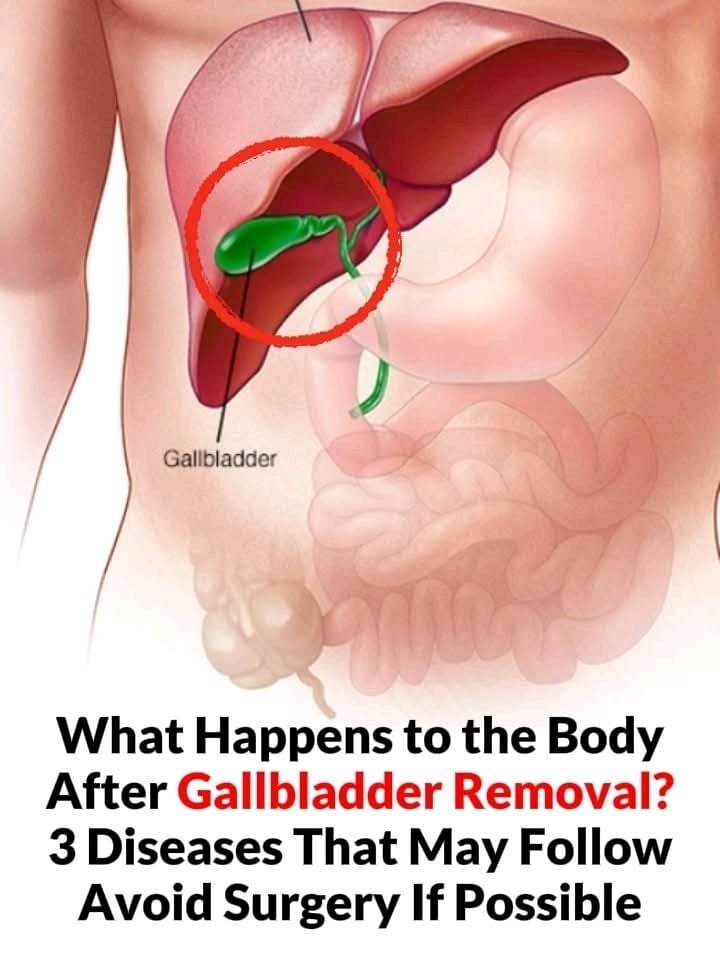
What Happens to the Body After Gallbladder Removal? 3 Diseases That May Follow – Avoid Surgery If Possible
The gallbladder is a small organ with a big role: storing and releasing bile, which helps digest fats. While gallbladder removal (cholecystectomy) is a common surgery, it is not without consequences. Understanding what happens to your body after gallbladder removal and the potential long-term effects can help you make informed decisions and possibly avoid surgery through alternative treatments.
1. The Role of the Gallbladder in the Body
The gallbladder:
-
Stores bile produced by the liver
-
Releases bile into the small intestine to digest fats
-
Supports absorption of fat-soluble vitamins (A, D, E, K)
When the gallbladder is removed:
-
Bile flows directly from the liver into the small intestine
-
The continuous flow can affect fat digestion
-
Some people develop long-term digestive issues
2. Changes in Digestion After Gallbladder Removal
Many patients experience digestive changes after surgery, such as:
-
Diarrhea and loose stools – The liver produces bile continuously, which can irritate the intestines.
-
Bloating and gas – Fat digestion is less efficient.
-
Difficulty digesting fatty meals – Greasy foods may trigger discomfort.
These symptoms are often mild, but in some cases, they can persist long-term.
3. Diseases That May Develop After Gallbladder Removal
While gallbladder removal can be life-saving for gallstones or infection, some conditions may arise post-surgery:
a. Fatty Liver Disease
-
Without the gallbladder regulating bile, fat metabolism in the liver can be disrupted.
-
Increased fat accumulation in liver cells can lead to non-alcoholic fatty liver disease (NAFLD).
-
Symptoms include fatigue, mild abdominal discomfort, and elevated liver enzymes.
Prevention tips:
-
Eat a low-fat, balanced diet
-
Exercise regularly
-
Monitor liver health with routine blood tests
b. Gastroesophageal Reflux Disease (GERD)
-
Direct bile flow into the intestines can sometimes reflux into the stomach and esophagus.
-
Symptoms: heartburn, regurgitation, chest discomfort.
-
Can lead to esophageal irritation or ulcers if unmanaged.
Management strategies:
-
Eat smaller meals and avoid lying down after eating
-
Limit spicy, fatty, and acidic foods
-
Consult a doctor for medications like antacids or proton pump inhibitors
c. Chronic Diarrhea or Irritable Bowel Syndrome (IBS)
-
Some patients experience bile acid diarrhea, which can mimic IBS.
-
Frequent, loose stools can occur for months or even years post-surgery.
Tips to reduce symptoms:
-
Limit high-fat meals
-
Eat smaller, more frequent meals
-
Use bile acid binders if prescribed by a doctor
4. When Surgery Can Be Avoided
Gallbladder removal is not always the only solution. Non-surgical options may include:
-
Dietary adjustments – Avoiding fatty, fried, and processed foods
-
Herbal remedies – Milk thistle, dandelion root, or artichoke extract (under guidance)
-
Medications – Ursodeoxycholic acid to dissolve small gallstones
-
Lifestyle changes – Maintaining a healthy weight and exercising regularly
Surgery should be a last resort when gallstones or complications are severe.
5. Tips for Protecting Your Body After Gallbladder Removal
-
Adopt a low-fat diet – Focus on lean proteins, vegetables, and whole grains.
-
Eat smaller, frequent meals – Reduces digestive stress.
-
Stay hydrated – Helps bile flow and digestion.
-
Include fiber gradually – Prevents diarrhea without causing bloating.
-
Monitor symptoms – Report persistent digestive issues to your doctor.
6. Conclusion
Gallbladder removal can relieve pain and prevent acute complications, but it may also trigger digestive issues and diseases like fatty liver, GERD, and chronic diarrhea. Whenever possible:
-
Explore dietary and lifestyle solutions first
-
Use non-surgical treatments under medical guidance
-
Stay aware of long-term digestive health after surgery
🩺 Pro Tip: Before deciding on gallbladder removal, ask your doctor about all alternatives, monitor your symptoms closely, and focus on preventive care to reduce risks.